- Getting Pregnant
- Registry Builder
- Baby Products
- Birth Clubs
- See all in Community
- Ovulation Calculator
- How To Get Pregnant
- How To Get Pregnant Fast
- Ovulation Discharge
- Implantation Bleeding
- Ovulation Symptoms
- Pregnancy Symptoms
- Am I Pregnant?
- Pregnancy Tests
- See all in Getting Pregnant
- Due Date Calculator
- Pregnancy Week by Week
- Pregnant Sex
- Weight Gain Tracker
- Signs of Labor
- Morning Sickness
- COVID Vaccine and Pregnancy
- Fetal Weight Chart
- Fetal Development
- Pregnancy Discharge
- Find Out Baby Gender
- Chinese Gender Predictor
- See all in Pregnancy
- Baby Name Generator
- Top Baby Names 2023
- Top Baby Names 2024
- How to Pick a Baby Name
- Most Popular Baby Names
- Baby Names by Letter
- Gender Neutral Names
- Unique Boy Names
- Unique Girl Names
- Top baby names by year
- See all in Baby Names
- Baby Development
- Baby Feeding Guide
- Newborn Sleep
- When Babies Roll Over
- First-Year Baby Costs Calculator
- Postpartum Health
- Baby Poop Chart
- See all in Baby
- Average Weight & Height
- Autism Signs
- Child Growth Chart
- Night Terrors
- Moving from Crib to Bed
- Toddler Feeding Guide
- Potty Training
- Bathing and Grooming
- See all in Toddler
- Height Predictor
- Potty Training: Boys
- Potty training: Girls
- How Much Sleep? (Ages 3+)
- Ready for Preschool?
- Thumb-Sucking
- Gross Motor Skills
- Napping (Ages 2 to 3)
- See all in Child
- Photos: Rashes & Skin Conditions
- Symptom Checker
- Vaccine Scheduler
- Reducing a Fever
- Acetaminophen Dosage Chart
- Constipation in Babies
- Ear Infection Symptoms
- Head Lice 101
- See all in Health
- Second Pregnancy
- Daycare Costs
- Family Finance
- Stay-At-Home Parents
- Breastfeeding Positions
- See all in Family
- Baby Sleep Training
- Preparing For Baby
- My Custom Checklist
- My Registries
- Take the Quiz
- Best Baby Products
- Best Breast Pump
- Best Convertible Car Seat
- Best Infant Car Seat
- Best Baby Bottle
- Best Baby Monitor
- Best Stroller
- Best Diapers
- Best Baby Carrier
- Best Diaper Bag
- Best Highchair
- See all in Baby Products
- Why Pregnant Belly Feels Tight
- Early Signs of Twins
- Teas During Pregnancy
- Baby Head Circumference Chart
- How Many Months Pregnant Am I
- What is a Rainbow Baby
- Braxton Hicks Contractions
- HCG Levels By Week
- When to Take a Pregnancy Test
- Am I Pregnant
- Why is Poop Green
- Can Pregnant Women Eat Shrimp
- Insemination
- UTI During Pregnancy
- Vitamin D Drops
- Best Baby Forumla
- Postpartum Depression
- Low Progesterone During Pregnancy
- Baby Shower
- Baby Shower Games

Cephalic presentation at 20 weeks
10 comments.
- s Shiza66 Original Poster Posted 07-14-23 TaviaLove said: No, it isn't too early. Baby still has plenty of room and time to chan… I was worried so, thanks ♥️
- s Shiza66 Original Poster Posted 07-15-23 TaviaLove said: Thank you and same to you! Do you feel heaviness in abdomen and pulse like feeling might be baby hiccups down there too because of cephalic presentation throughout?
- t TaviaLove Posted 07-15-23 If you have concerns, feel free to call the doctor or go to L&D.
- s Shiza66 Original Poster Posted 07-15-23 TaviaLove said: I feel heaviness down low after a long day or a lot of walking. Pulse … Yup exactly I feel the same
- t TaviaLove Posted 07-15-23 It sounds like we're both good 😊
Where to go next

Appointments at Mayo Clinic
- Pregnancy week by week
- Fetal presentation before birth
The way a baby is positioned in the uterus just before birth can have a big effect on labor and delivery. This positioning is called fetal presentation.
Babies twist, stretch and tumble quite a bit during pregnancy. Before labor starts, however, they usually come to rest in a way that allows them to be delivered through the birth canal headfirst. This position is called cephalic presentation. But there are other ways a baby may settle just before labor begins.
Following are some of the possible ways a baby may be positioned at the end of pregnancy.
Head down, face down
When a baby is head down, face down, the medical term for it is the cephalic occiput anterior position. This the most common position for a baby to be born in. With the face down and turned slightly to the side, the smallest part of the baby's head leads the way through the birth canal. It is the easiest way for a baby to be born.
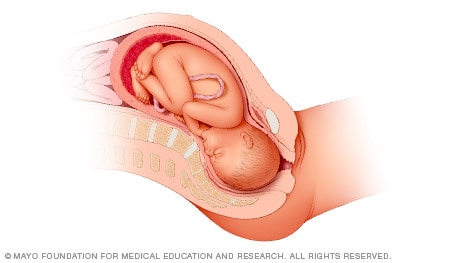
Head down, face up
When a baby is head down, face up, the medical term for it is the cephalic occiput posterior position. In this position, it might be harder for a baby's head to go under the pubic bone during delivery. That can make labor take longer.
Most babies who begin labor in this position eventually turn to be face down. If that doesn't happen, and the second stage of labor is taking a long time, a member of the health care team may reach through the vagina to help the baby turn. This is called manual rotation.
In some cases, a baby can be born in the head-down, face-up position. Use of forceps or a vacuum device to help with delivery is more common when a baby is in this position than in the head-down, face-down position. In some cases, a C-section delivery may be needed.
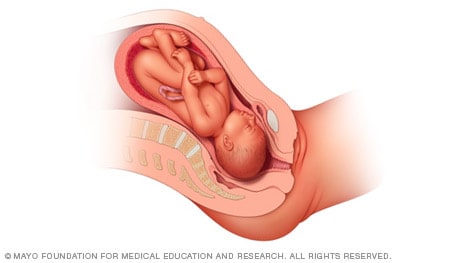
Frank breech
When a baby's feet or buttocks are in place to come out first during birth, it's called a breech presentation. This happens in about 3% to 4% of babies close to the time of birth. The baby shown below is in a frank breech presentation. That's when the knees aren't bent, and the feet are close to the baby's head. This is the most common type of breech presentation.
If you are more than 36 weeks into your pregnancy and your baby is in a frank breech presentation, your health care professional may try to move the baby into a head-down position. This is done using a procedure called external cephalic version. It involves one or two members of the health care team putting pressure on your belly with their hands to get the baby to roll into a head-down position.
If the procedure isn't successful, or if the baby moves back into a breech position, talk with a member of your health care team about the choices you have for delivery. Most babies in a frank breech position are born by planned C-section.

Complete and incomplete breech
A complete breech presentation, as shown below, is when the baby has both knees bent and both legs pulled close to the body. In an incomplete breech, one or both of the legs are not pulled close to the body, and one or both of the feet or knees are below the baby's buttocks. If a baby is in either of these positions, you might feel kicking in the lower part of your belly.
If you are more than 36 weeks into your pregnancy and your baby is in a complete or incomplete breech presentation, your health care professional may try to move the baby into a head-down position. This is done using a procedure called external cephalic version. It involves one or two members of the health care team putting pressure on your belly with their hands to get the baby to roll into a head-down position.
If the procedure isn't successful, or if the baby moves back into a breech position, talk with a member of your health care team about the choices you have for delivery. Many babies in a complete or incomplete breech position are born by planned C-section.

When a baby is sideways — lying horizontal across the uterus, rather than vertical — it's called a transverse lie. In this position, the baby's back might be:
- Down, with the back facing the birth canal.
- Sideways, with one shoulder pointing toward the birth canal.
- Up, with the hands and feet facing the birth canal.
Although many babies are sideways early in pregnancy, few stay this way when labor begins.
If your baby is in a transverse lie during week 37 of your pregnancy, your health care professional may try to move the baby into a head-down position. This is done using a procedure called external cephalic version. External cephalic version involves one or two members of your health care team putting pressure on your belly with their hands to get the baby to roll into a head-down position.
If the procedure isn't successful, or if the baby moves back into a transverse lie, talk with a member of your health care team about the choices you have for delivery. Many babies who are in a transverse lie are born by C-section.
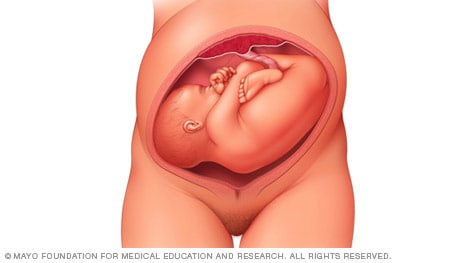
If you're pregnant with twins and only the twin that's lower in the uterus is head down, as shown below, your health care provider may first deliver that baby vaginally.
Then, in some cases, your health care team may suggest delivering the second twin in the breech position. Or they may try to move the second twin into a head-down position. This is done using a procedure called external cephalic version. External cephalic version involves one or two members of the health care team putting pressure on your belly with their hands to get the baby to roll into a head-down position.
Your health care team may suggest delivery by C-section for the second twin if:
- An attempt to deliver the baby in the breech position is not successful.
- You do not want to try to have the baby delivered vaginally in the breech position.
- An attempt to move the baby into a head-down position is not successful.
- You do not want to try to move the baby to a head-down position.
In some cases, your health care team may advise that you have both twins delivered by C-section. That might happen if the lower twin is not head down, the second twin has low or high birth weight as compared to the first twin, or if preterm labor starts.
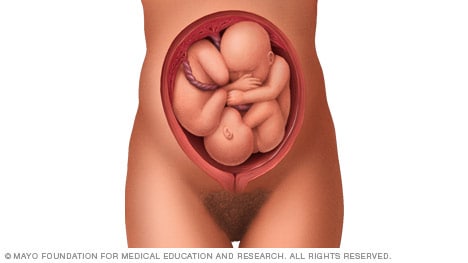
- Landon MB, et al., eds. Normal labor and delivery. In: Gabbe's Obstetrics: Normal and Problem Pregnancies. 8th ed. Elsevier; 2021. https://www.clinicalkey.com. Accessed May 19, 2023.
- Holcroft Argani C, et al. Occiput posterior position. https://www.updtodate.com/contents/search. Accessed May 19, 2023.
- Frequently asked questions: If your baby is breech. American College of Obstetricians and Gynecologists https://www.acog.org/womens-health/faqs/if-your-baby-is-breech. Accessed May 22, 2023.
- Hofmeyr GJ. Overview of breech presentation. https://www.updtodate.com/contents/search. Accessed May 22, 2023.
- Strauss RA, et al. Transverse fetal lie. https://www.updtodate.com/contents/search. Accessed May 22, 2023.
- Chasen ST, et al. Twin pregnancy: Labor and delivery. https://www.updtodate.com/contents/search. Accessed May 22, 2023.
- Cohen R, et al. Is vaginal delivery of a breech second twin safe? A comparison between delivery of vertex and non-vertex second twins. The Journal of Maternal-Fetal & Neonatal Medicine. 2021; doi:10.1080/14767058.2021.2005569.
- Marnach ML (expert opinion). Mayo Clinic. May 31, 2023.
Products and Services
- A Book: Obstetricks
- A Book: Mayo Clinic Guide to a Healthy Pregnancy
- 3rd trimester pregnancy
- Fetal development: The 3rd trimester
- Overdue pregnancy
- Pregnancy due date calculator
- Prenatal care: 3rd trimester
Mayo Clinic does not endorse companies or products. Advertising revenue supports our not-for-profit mission.
- Opportunities
Mayo Clinic Press
Check out these best-sellers and special offers on books and newsletters from Mayo Clinic Press .
- Mayo Clinic on Incontinence - Mayo Clinic Press Mayo Clinic on Incontinence
- The Essential Diabetes Book - Mayo Clinic Press The Essential Diabetes Book
- Mayo Clinic on Hearing and Balance - Mayo Clinic Press Mayo Clinic on Hearing and Balance
- FREE Mayo Clinic Diet Assessment - Mayo Clinic Press FREE Mayo Clinic Diet Assessment
- Mayo Clinic Health Letter - FREE book - Mayo Clinic Press Mayo Clinic Health Letter - FREE book
- Healthy Lifestyle
Your gift holds great power – donate today!
Make your tax-deductible gift and be a part of the cutting-edge research and care that's changing medicine.
- Type 2 Diabetes
- Heart Disease
- Digestive Health
- Multiple Sclerosis
- Diet & Nutrition
- Supplements
- Health Insurance
- Public Health
- Patient Rights
- Caregivers & Loved Ones
- End of Life Concerns
- Health News
- Thyroid Test Analyzer
- Doctor Discussion Guides
- Hemoglobin A1c Test Analyzer
- Lipid Test Analyzer
- Complete Blood Count (CBC) Analyzer
- What to Buy
- Editorial Process
- Meet Our Medical Expert Board
What Is Cephalic Position?
The ideal fetal position for labor and delivery
- Why It's Best
Risks of Other Positions
- Determining Position
- Turning a Fetus
The cephalic position is when a fetus is head down when it is ready to enter the birth canal. This is one of a few variations of how a fetus can rest in the womb and is considered the ideal one for labor and delivery.
About 96% of babies are born in the cephalic position. Most settle into it between the 32nd and 36th weeks of pregnancy . Your healthcare provider will monitor the fetus's position during the last weeks of gestation to ensure this has happened by week 36.
If the fetus is not in the cephalic position at that point, the provider may try to turn it. If this doesn't work, some—but not all—practitioners will attempt to deliver vaginally, while others will recommend a Cesarean (C-section).
Getty Images
Why Is the Cephalic Position Best?
During labor, contractions dilate the cervix so the fetus has adequate room to come through the birth canal. The cephalic position is the easiest and safest way for the baby to pass through the birth canal.
If the fetus is in a noncephalic position, delivery becomes more challenging. Different fetal positions have a range of difficulties and varying risks.
A small percentage of babies present in noncephalic positions. This can pose risks both to the fetus and the mother, and make labor and delivery more challenging. It can also influence the way in which someone can deliver.
A fetus may actually find itself in any of these positions throughout pregnancy, as the move about the uterus. But as they grow, there will be less room to tumble around and they will settle into a final position.
It is at this point that noncephalic positions can pose significant risks.
Cephalic Posterior
A fetus may also present in an occiput or cephalic posterior position. This means they are positioned head down, but they are facing the abdomen instead of the back.
This position is also nicknamed "sunny-side up."
Presenting this way increases the chance of a painful and prolonged delivery.
There are three different types of breech fetal positioning:
- Frank breech: The legs are up with the feet near the head.
- Footling breech: One or both legs is lowered over the cervix.
- Complete breech: The fetus is bottom-first with knees bent.
A vaginal delivery is most times a safe way to deliver. But with breech positions, a vaginal delivery can be complicated.
When a baby is born in the breech position, the largest part—its head—is delivered last. This can result in them getting stuck in the birth canal (entrapped). This can cause injury or death.
The umbilical cord may also be damaged or slide down into the mouth of the womb, which can reduce or cut off the baby's oxygen supply.
Some providers are still comfortable performing a vaginal birth as long as the fetus is doing well. But breech is always a riskier delivery position compared with the cephalic position, and most cases require a C-section.
Likelihood of a Breech Baby
You are more likely to have a breech baby if you:
- Go into early labor before you're full term
- Have an abnormally shaped uterus, fibroids , or too much amniotic fluid
- Are pregnant with multiples
- Have placenta previa (when the placenta covers the cervix)
Transverse Lie
In transverse lie position, the fetus is presenting sideways across the uterus rather than vertically. They may be:
- Down, with the back facing the birth canal
- With one shoulder pointing toward the birth canal
- Up, with the hands and feet facing the birth canal
If a transverse lie is not corrected before labor, a C-section will be required. This is typically the case.
Determining Fetal Position
Your healthcare provider can determine if your baby is in cephalic presentation by performing a physical exam and ultrasound.
In the final weeks of pregnancy, your healthcare provider will feel your lower abdomen with their hands to assess the positioning of the baby. This includes where the head, back, and buttocks lie
If your healthcare provider senses that the fetus is in a breech position, they can use ultrasound to confirm their suspicion.
Turning a Fetus So They Are in Cephalic Position
External cephalic version (ECV) is a common, noninvasive procedure to turn a breech baby into cephalic position while it's still in the uterus.
This is only considered if a healthcare provider monitors presentation progress in the last trimester and notices that a fetus is maintaining a noncephalic position as your delivery date approaches.
External Cephalic Version (ECV)
ECV involves the healthcare provider applying pressure to your stomach to turn the fetus from the outside. They will attempt to rotate the head forward or backward and lift the buttocks in an upward position. Sometimes, they use ultrasound to help guide the process.
The best time to perform ECV is about 37 weeks of pregnancy. Afterward, the fetal heart rate will be monitored to make sure it’s within normal levels. You should be able to go home after having ECV done.
ECV has a 50% to 60% success rate. However, even if it does work, there is still a chance the fetus will return to the breech position before birth.
Natural Methods For Turning a Fetus
There are also natural methods that can help turn a fetus into cephalic position. There is no medical research that confirms their efficacy, however.
- Changing your position: Sometimes a fetus will move when you get into certain positions. Two specific movements that your provider may recommend include: Getting on your hands and knees and gently rocking back and forth. Another you could try is pushing your hips up in the air while laying on your back with your knees bent and feet flat on the floor (bridge pose).
- Playing stimulating sounds: Fetuses gravitate to sound. You may be successful at luring a fetus out of breech position by playing music or a recording of your voice near your lower abdomen.
- Chiropractic care: A chiropractor can try the Webster technique. This is a specific chiropractic analysis and adjustment which enables chiropractors to establish balance in the pregnant person's pelvis and reduce undue stress to the uterus and supporting ligaments.
- Acupuncture: This is a considerably safe way someone can try to turn a fetus. Some practitioners incorporate moxibustion—the burning of dried mugwort on certain areas of the body—because they believe it will enhance the chances of success.
A Word From Verywell
While most babies are born in cephalic position at delivery, this is not always the case. And while some fetuses can be turned, others may be more stubborn.
This may affect your labor and delivery wishes. Try to remember that having a healthy baby, and staying well yourself, are your ultimate priorities. That may mean diverting from your best laid plans.
Speaking to your healthcare provider about turning options and the safest route of delivery may help you adjust to this twist and feel better about how you will move ahead.
Glezerman M. Planned vaginal breech delivery: current status and the need to reconsider . Expert Rev Obstet Gynecol. 2012;7(2):159-166. doi:10.1586/eog.12.2
Cleveland Clinic. Fetal positions for birth .
MedlinePlus. Breech birth .
UT Southwestern Medical Center. Can you turn a breech baby around?
The American College of Obstetricians and Gynecologists. If your baby is breech .
Roecker CB. Breech repositioning unresponsive to Webster technique: coexistence of oligohydramnios . Journal of Chiropractic Medicine . 2013;12(2):74-78. doi:10.1016/j.jcm.2013.06.003
By Cherie Berkley, MS Berkley is a journalist with a certification in global health from Johns Hopkins University and a master's degree in journalism.
Need to talk? Call 1800 882 436. It's a free call with a maternal child health nurse. *call charges may apply from your mobile
Is it an emergency? Dial 000 If you need urgent medical help, call triple zero immediately.
Share via email
There is a total of 5 error s on this form, details are below.
- Please enter your name
- Please enter your email
- Your email is invalid. Please check and try again
- Please enter recipient's email
- Recipient's email is invalid. Please check and try again
- Agree to Terms required
Error: This is required
Error: Not a valid value
Presentation and position of baby through pregnancy and at birth
9-minute read
If you are concerned about your baby’s movements, contact your doctor or midwife for advice immediately.
- If you baby is in a breech presentation, your doctor may recommend trying a technique called an external cephalic version to try and move your baby while they are still in the uterus for an easier birth.
What does presentation and position mean?
Presentation refers to the part of your baby’s body that is facing downwards in the direction of the birth canal.
Position refers to where your baby’s occiput (the bottom part of the back of their head) is in relation to your body.
If your baby is in a breech presentation , then position refers to where your baby’s sacrum (lower back) is in relation to your body.
People — including medical professionals — sometimes use these terms incorrectly. Sometimes when speaking about babies in breech presentation, the word ‘position’ will be used to refer to their presentation. For example, you may read information or hear people say ‘breech position’ instead of ‘breech presentation’.
What are the different types of presentation my baby could be in during pregnancy and birth?
Most babies present headfirst, also known as cephalic presentation. Most babies that are headfirst will be vertex presentation. This means that the crown of their head sits at the opening of your birth canal.
In rare cases, your baby can be headfirst but in face or brow presentation, which may not be suitable for vaginal birth.

If your baby is in a breech presentation, their feet or bottom will be closest to your birth canal. The 3 most common types of breech presentation are:
- frank or extended breech — where your baby’s legs are straight up in front of their body, with their feet up near their face
- complete or flexed breech — where your baby is in a sitting position with their legs crossed in front of their body and their feet near their bottom
- footling breech — where one or both of your baby’s feet are hanging below their bottom, so the foot or feet are coming first
Read more on breech presentation .
What are the different positions my baby could be in during pregnancy and birth?
If your baby is headfirst, the 3 main types of presentation are:
- anterior – when the back of your baby’s head is at the front of your belly
- lateral – when the back of your baby’s head is facing your side
- posterior – when the back of your baby’s head is towards your back

How will I know what presentation and position my baby is in?
Your doctor or midwife can usually work out your baby’s presentation by feeling your abdomen. They may also double check it with a portable ultrasound. Your baby’s presentation is usually checked around 36 weeks .
Your doctor or midwife will also confirm your baby’s head position in labour by examining your belly and using an ultrasound , and they may also do a vaginal examination . During the vaginal examination they are feeling for certain ridges on your baby’s head called sutures and fontanelles that help them work out which way your baby is positioned.
What is the ideal presentation and position for baby to be in for a vaginal birth?
For a vaginal birth, your baby will ideally be headfirst with the back of their head at the front of your belly, also known as being in the anterior position. This position is best for labour and birth since it means that the smallest part of your baby’s head goes down the birth canal first.

When does a baby usually get in the ideal presentation and position for birth?
Your baby will usually be in a headfirst position by 37 weeks of pregnancy. Around 3 in every 100 babies will be in breech presentation after 37 weeks.
Your baby’s position can change with your contractions during labour as they move down the birth canal, so their exact position can change during labour.
What are my options if baby isn't in the ideal presentation or position for a vaginal birth?
If your baby is in a breech presentation, your doctor may recommend a technique called an external cephalic version (ECV) to try and move your baby while they are still in the uterus . An ECV involves your doctor using their hands to apply pressure on your belly and help turn your baby to a headfirst position. It has a 1 in 2 chance of success and is a safe option in most pregnancies.
There is no evidence to show that alternative therapies, such as exercises, acupuncture or chiropractic treatments, help your baby change from a breech presentation to headfirst.
If your baby remains breech, your doctor may discuss having a breech vaginal birth. Not all doctors and hospitals offer this option. They may also suggest you birth your baby with a planned caesarean section .
If your baby’s presentation is headfirst but the position of your baby’s head is not ideal for labour, it can lead to a longer labour, and potential complications . The position of your baby’s head will often change as your labour progresses. If it doesn’t, sometimes you can still give birth without assistance, or you may need your doctor to help turn your baby’s head or help your birth with a vacuum or forceps .
Any procedure or decision for a type of birth will only go ahead with your consent . You will be able to discuss all the options with your doctor, and based on your preferences for yourself and your baby’s safety, make a decision together .
Resources and support
The Royal Australian and New Zealand College of Obstetrics and Gynaecology has a factsheet about the options available to you if your baby is in a breech presentation at the end of your pregnancy .
Mercy Perinatal has information on external cephalic version (ECV) safety and benefits if your baby is in a breech presentation at the end of your pregnancy.
The Women’s Hospital has information about the different presentations and positions your baby could be in, and how it can affect your birthing experience.

Speak to a maternal child health nurse
Call Pregnancy, Birth and Baby to speak to a maternal child health nurse on 1800 882 436 or video call . Available 7am to midnight (AET), 7 days a week.
Learn more here about the development and quality assurance of healthdirect content .
Last reviewed: October 2023
Related pages
External cephalic version (ecv), malpresentation, breech pregnancy, search our site for.
- Foetal Version
- Breech Presentation
Need more information?
Top results
Breech presentation and turning the baby
In preparation for a safe birth, your health team will need to turn your baby if it is in a bottom first ‘breech’ position.
Read more on WA Health website


Breech Presentation at the End of your Pregnancy
Breech presentation occurs when your baby is lying bottom first or feet first in the uterus (womb) rather than the usual head first position. In early pregnancy, a breech position is very common.
Read more on RANZCOG - Royal Australian and New Zealand College of Obstetricians and Gynaecologists website

External Cephalic Version for Breech Presentation - Pregnancy and the first five years
This information brochure provides information about an External Cephalic Version (ECV) for breech presentation
Read more on NSW Health website

When a baby is positioned bottom-down late in pregnancy, this is called the breech position. Find out about 3 main types and safe birthing options.
Read more on Pregnancy, Birth & Baby website

Malpresentation is when your baby is in an unusual position as the birth approaches. Sometimes it’s possible to move the baby, but a caesarean maybe safer.
Labour complications
Even if you’re healthy and well prepared for childbirth, there’s always a chance of unexpected problems. Learn more about labour complications.
ECV is a procedure to try to move your baby from a breech position to a head-down position. This is performed by a trained doctor.
Having a baby
The articles in this section relate to having a baby – what to consider before becoming pregnant, pregnancy and birth, and after your baby is born.
Anatomy of pregnancy and birth - pelvis
Your pelvis helps to carry your growing baby and is tailored for vaginal births. Learn more about the structure and function of the female pelvis.
Planned or elective caesarean
There are important things to consider if you are having a planned or elective caesarean such as what happens during and after the procedure.
Pregnancy, Birth and Baby is not responsible for the content and advertising on the external website you are now entering.
Call us and speak to a Maternal Child Health Nurse for personal advice and guidance.
Need further advice or guidance from our maternal child health nurses?
1800 882 436
Government Accredited with over 140 information partners
We are a government-funded service, providing quality, approved health information and advice

Healthdirect Australia acknowledges the Traditional Owners of Country throughout Australia and their continuing connection to land, sea and community. We pay our respects to the Traditional Owners and to Elders both past and present.
© 2024 Healthdirect Australia Limited
This information is for your general information and use only and is not intended to be used as medical advice and should not be used to diagnose, treat, cure or prevent any medical condition, nor should it be used for therapeutic purposes.
The information is not a substitute for independent professional advice and should not be used as an alternative to professional health care. If you have a particular medical problem, please consult a healthcare professional.
Except as permitted under the Copyright Act 1968, this publication or any part of it may not be reproduced, altered, adapted, stored and/or distributed in any form or by any means without the prior written permission of Healthdirect Australia.
Support this browser is being discontinued for Pregnancy, Birth and Baby
Support for this browser is being discontinued for this site
- Internet Explorer 11 and lower
We currently support Microsoft Edge, Chrome, Firefox and Safari. For more information, please visit the links below:
- Chrome by Google
- Firefox by Mozilla
- Microsoft Edge
- Safari by Apple
You are welcome to continue browsing this site with this browser. Some features, tools or interaction may not work correctly.
- Getting Pregnant
- Registry Builder
- Baby Products
- Birth Clubs
- See all in Community
- Ovulation Calculator
- How To Get Pregnant
- How To Get Pregnant Fast
- Ovulation Discharge
- Implantation Bleeding
- Ovulation Symptoms
- Pregnancy Symptoms
- Am I Pregnant?
- Pregnancy Tests
- See all in Getting Pregnant
- Due Date Calculator
- Pregnancy Week by Week
- Pregnant Sex
- Weight Gain Tracker
- Signs of Labor
- Morning Sickness
- COVID Vaccine and Pregnancy
- Fetal Weight Chart
- Fetal Development
- Pregnancy Discharge
- Find Out Baby Gender
- Chinese Gender Predictor
- See all in Pregnancy
- Baby Name Generator
- Top Baby Names 2023
- Top Baby Names 2024
- How to Pick a Baby Name
- Most Popular Baby Names
- Baby Names by Letter
- Gender Neutral Names
- Unique Boy Names
- Unique Girl Names
- Top baby names by year
- See all in Baby Names
- Baby Development
- Baby Feeding Guide
- Newborn Sleep
- When Babies Roll Over
- First-Year Baby Costs Calculator
- Postpartum Health
- Baby Poop Chart
- See all in Baby
- Average Weight & Height
- Autism Signs
- Child Growth Chart
- Night Terrors
- Moving from Crib to Bed
- Toddler Feeding Guide
- Potty Training
- Bathing and Grooming
- See all in Toddler
- Height Predictor
- Potty Training: Boys
- Potty training: Girls
- How Much Sleep? (Ages 3+)
- Ready for Preschool?
- Thumb-Sucking
- Gross Motor Skills
- Napping (Ages 2 to 3)
- See all in Child
- Photos: Rashes & Skin Conditions
- Symptom Checker
- Vaccine Scheduler
- Reducing a Fever
- Acetaminophen Dosage Chart
- Constipation in Babies
- Ear Infection Symptoms
- Head Lice 101
- See all in Health
- Second Pregnancy
- Daycare Costs
- Family Finance
- Stay-At-Home Parents
- Breastfeeding Positions
- See all in Family
- Baby Sleep Training
- Preparing For Baby
- My Custom Checklist
- My Registries
- Take the Quiz
- Best Baby Products
- Best Breast Pump
- Best Convertible Car Seat
- Best Infant Car Seat
- Best Baby Bottle
- Best Baby Monitor
- Best Stroller
- Best Diapers
- Best Baby Carrier
- Best Diaper Bag
- Best Highchair
- See all in Baby Products
- Why Pregnant Belly Feels Tight
- Early Signs of Twins
- Teas During Pregnancy
- Baby Head Circumference Chart
- How Many Months Pregnant Am I
- What is a Rainbow Baby
- Braxton Hicks Contractions
- HCG Levels By Week
- When to Take a Pregnancy Test
- Am I Pregnant
- Why is Poop Green
- Can Pregnant Women Eat Shrimp
- Insemination
- UTI During Pregnancy
- Vitamin D Drops
- Best Baby Forumla
- Postpartum Depression
- Low Progesterone During Pregnancy
- Baby Shower
- Baby Shower Games
Breech, posterior, transverse lie: What position is my baby in?

Fetal presentation, or how your baby is situated in your womb at birth, is determined by the body part that's positioned to come out first, and it can affect the way you deliver. At the time of delivery, 97 percent of babies are head-down (cephalic presentation). But there are several other possibilities, including feet or bottom first (breech) as well as sideways (transverse lie) and diagonal (oblique lie).
Fetal presentation and position
During the last trimester of your pregnancy, your provider will check your baby's presentation by feeling your belly to locate the head, bottom, and back. If it's unclear, your provider may do an ultrasound or an internal exam to feel what part of the baby is in your pelvis.
Fetal position refers to whether the baby is facing your spine (anterior position) or facing your belly (posterior position). Fetal position can change often: Your baby may be face up at the beginning of labor and face down at delivery.
Here are the many possibilities for fetal presentation and position in the womb.
Medical illustrations by Jonathan Dimes
Head down, facing down (anterior position)
A baby who is head down and facing your spine is in the anterior position. This is the most common fetal presentation and the easiest position for a vaginal delivery.
This position is also known as "occiput anterior" because the back of your baby's skull (occipital bone) is in the front (anterior) of your pelvis.
Head down, facing up (posterior position)
In the posterior position , your baby is head down and facing your belly. You may also hear it called "sunny-side up" because babies who stay in this position are born facing up. But many babies who are facing up during labor rotate to the easier face down (anterior) position before birth.
Posterior position is formally known as "occiput posterior" because the back of your baby's skull (occipital bone) is in the back (posterior) of your pelvis.
Frank breech
In the frank breech presentation, both the baby's legs are extended so that the feet are up near the face. This is the most common type of breech presentation. Breech babies are difficult to deliver vaginally, so most arrive by c-section .
Some providers will attempt to turn your baby manually to the head down position by applying pressure to your belly. This is called an external cephalic version , and it has a 58 percent success rate for turning breech babies. For more information, see our article on breech birth .
Complete breech
A complete breech is when your baby is bottom down with hips and knees bent in a tuck or cross-legged position. If your baby is in a complete breech, you may feel kicking in your lower abdomen.
Incomplete breech
In an incomplete breech, one of the baby's knees is bent so that the foot is tucked next to the bottom with the other leg extended, positioning that foot closer to the face.
Single footling breech
In the single footling breech presentation, one of the baby's feet is pointed toward your cervix.
Double footling breech
In the double footling breech presentation, both of the baby's feet are pointed toward your cervix.
Transverse lie
In a transverse lie, the baby is lying horizontally in your uterus and may be facing up toward your head or down toward your feet. Babies settle this way less than 1 percent of the time, but it happens more commonly if you're carrying multiples or deliver before your due date.
If your baby stays in a transverse lie until the end of your pregnancy, it can be dangerous for delivery. Your provider will likely schedule a c-section or attempt an external cephalic version , which is highly successful for turning babies in this position.
Oblique lie
In rare cases, your baby may lie diagonally in your uterus, with his rump facing the side of your body at an angle.
Like the transverse lie, this position is more common earlier in pregnancy, and it's likely your provider will intervene if your baby is still in the oblique lie at the end of your third trimester.
Was this article helpful?
What to know if your baby is breech

What's a sunny-side up baby?

What happens to your baby right after birth

How your twins’ fetal positions affect labor and delivery

BabyCenter's editorial team is committed to providing the most helpful and trustworthy pregnancy and parenting information in the world. When creating and updating content, we rely on credible sources: respected health organizations, professional groups of doctors and other experts, and published studies in peer-reviewed journals. We believe you should always know the source of the information you're seeing. Learn more about our editorial and medical review policies .
Ahmad A et al. 2014. Association of fetal position at onset of labor and mode of delivery: A prospective cohort study. Ultrasound in obstetrics & gynecology 43(2):176-182. https://www.ncbi.nlm.nih.gov/pubmed/23929533 Opens a new window [Accessed September 2021]
Gray CJ and Shanahan MM. 2019. Breech presentation. StatPearls. https://www.ncbi.nlm.nih.gov/books/NBK448063/ Opens a new window [Accessed September 2021]
Hankins GD. 1990. Transverse lie. American Journal of Perinatology 7(1):66-70. https://www.ncbi.nlm.nih.gov/pubmed/2131781 Opens a new window [Accessed September 2021]
Medline Plus. 2020. Your baby in the birth canal. U.S. National Library of Medicine. https://medlineplus.gov/ency/article/002060.htm Opens a new window [Accessed September 2021]

Where to go next

An official website of the United States government
The .gov means it's official. Federal government websites often end in .gov or .mil. Before sharing sensitive information, make sure you're on a federal government site.
The site is secure. The https:// ensures that you are connecting to the official website and that any information you provide is encrypted and transmitted securely.
- Publications
- Account settings
- Browse Titles
NCBI Bookshelf. A service of the National Library of Medicine, National Institutes of Health.
StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2024 Jan-.

StatPearls [Internet].
External cephalic version.
Meaghan M. Shanahan ; Daniel J. Martingano ; Caron J. Gray .
Affiliations
Last Update: December 13, 2023 .
- Continuing Education Activity
In carefully selected patients, an external cephalic version (ECV) may be an alternative to cesarean delivery for fetal malpresentation at term. ECV is a noninvasive procedure that manipulates fetal position through the abdominal wall of the gravida. With the global cesarean section rate reaching 34%, fetal malpresentation ranks as the third most common indication for cesarean delivery, accounting for nearly 17% of cases. Studies suggest a 60% mean success rate for ECV, emphasizing its cost-effectiveness and potential to decrease cesarean delivery rates significantly. While particularly crucial in resource-limited settings where access to medical services during labor is constrained or cesarean delivery is unavailable or unsafe, ECV presents a viable option to improve rates of vaginal delivery in singleton gestations in all settings.
This activity reviews the indications, contraindications, necessary equipment, preferred personnel, procedural technique, risks, and benefits of ECV and highlights the role of the interprofessional team in caring for patients who may benefit from this procedure.
- Select suitable candidates for an external cephalic version based on their clinical history and presentation.
- Screen patients effectively regarding the risks and benefits of an external cephalic version.
- Apply best practices when performing an external cephalic version.
- Develop and implement effective interpersonal team strategies to improve outcomes for patients undergoing external cephalic version.
- Introduction
The global cesarean section rate has increased from approximately 23% to 34% in the past decade. Fetal malpresentation is now the third-most common indication for cesarean delivery, encompassing nearly 17% of cases. Almost one-fourth of all fetuses are in a breech presentation at 28 weeks gestational age; this number decreases to between 3% and 4% at term. In current clinical practice, most pregnancies with a breech fetus are delivered by cesarean section.
Individual and institutional efforts are increasing to reduce the overall cesarean delivery rate, particularly for nulliparous patients with term, singleton, and vertex gestations. [1] [2] An alternative to cesarean delivery for fetal malpresentation at term is an external cephalic version (ECV), a procedure to correct fetal malpresentation. ECV may be indicated when the fetus is breech or in an oblique or transverse lie after 37 0/7 weeks gestation. [3] The overall success rate for ECV approaches 60%, is cost-effective, and can lead to decreased cesarean delivery rates. [4] ECV is of particular importance in resource-poor environments, where patients may have limited access to medical services during labor and delivery or where cesarean delivery is unavailable or unsafe.
- Anatomy and Physiology
ECV can be attempted when managing breech presentations or fetuses with a transverse or oblique lie. Three types of breech presentation are established concerning fetal attitude: complete, frank, and incomplete, which is sometimes referred to as footling breech. In complete breech, the fetal pelvis engages with the maternal pelvic inlet, and the fetal hips and knees are flexed. In frank breech, the fetal pelvis engages with the maternal pelvic inlet, the fetal hips are flexed, the knees are extended, and the feet are near the head. In incomplete or footling breech, one (single footling) or both (double footling) feet are extended below the level of the fetal pelvis.
A fetus with a transverse lie is positioned with their long axis, defined as the spine, at a right angle to the long axis of the gravida. The fetal head may be to the right or left side of the maternal spine. The fetus may be facing up or down. The long axis of the fetus characterizes an oblique lie at any angle to the maternal long axis that is not 90°. An oblique fetus is usually positioned with their head in the right or left lower quadrants, although this is not universal.
- Indications
ECV may be indicated in carefully selected patients. The fetus must be at or beyond 36 0/7 weeks of gestation with malpresentation, and there must be no absolute contraindications to vaginal delivery, such as placenta previa, vasa previa, or a history of classical cesarean delivery. Fetal status must be reassuring, and preprocedural nonstress testing is recommended. While ECV may be performed as early as 36 0/7 weeks gestation, many practitioners will delay ECV until 37 0/7 weeks gestation to ensure delivery of a term fetus.
ECV is more successful in multigravidas, those with a complete breech or transverse or oblique presentation, an unengaged presenting part, adequate amniotic fluid, and a posterior placenta. Nulliparous patients and those with an anterior, lateral, or cornual placenta have lower success rates. Patients with advanced cervical dilatation, obesity, oligohydramnios, or ruptured membranes also have lower success rates. Additionally, if the fetus weighs less than 2500 g, is at a low station with an engaged presenting part, is frank breech, or the spine is posterior, the success of ECV is decreased. [5]
Evidence supports the use of parenteral tocolysis, most often with the beta-2-agonist medication terbutaline, to improve the success of ECV; most studies evaluating the various aspects of ECV aspects include using a tocolytic agent. [6] [7] [8] [9] Data regarding the improved success of ECV incorporating regional anesthesia is inconsistent.
- Contraindications
Any contraindication to vaginal delivery would also be a contraindication to ECV. These contraindications include but are not limited to placenta previa, vasa previa, active genital herpes outbreak, or a history of classical cesarean delivery. A history of low transverse cesarean delivery is not an absolute contraindication to ECV. [10] The overall success rate of ECV in patients with a previous cesarean birth ranges from 50% to 84%; no cases of uterine rupture during ECV were reported in the four trials evaluating this outcome in patients with a prior cesarean delivery. [11] [12] [13] [14]
Antepartum ECV is contraindicated in multiple gestations, although it can be utilized for twin gestations that would otherwise be suitable candidates for breech extraction. [15] [16]
Patients with severe oligohydramnios, nonreassuring fetal monitoring, a hyperextended fetal head, significant fetal or uterine anomaly, fetal growth restriction, and maternal hypertension carry a low likelihood of successful ECV and a significantly increased risk of poor fetal outcomes; ECV in such situations requires careful consideration.
If a gravida who is otherwise a suitable candidate for ECV presents in early labor with fetal malpresentation, ECV may be a reasonable option if the presenting part is unengaged, the amniotic fluid index is within the normal range, and there are no contraindications to ECV or vaginal delivery. Data from the Nationwide Inpatient Sample from 1998 to 2011 noted a success rate of 65% for ECV performed in carefully selected patients during the admission for delivery. [17] ECV performed in this circumstance resulted in a significantly lower cesarean birth rate and hospital stay of greater than 7 days compared to patients with a persistent breech presentation at the time of delivery. [17]
External cephalic versions should be attempted only in settings where cesarean delivery services are readily available. Therefore, the required equipment for ECV includes all such requirements for cesarean delivery, including anesthesia services. Access to tocolytic agents, bedside ultrasonography, and external fetal heart rate monitoring equipment is also required. Following ECV, fetal status must be assessed; nonstress testing is preferred. If nonstress testing is unavailable, Doppler indices of the umbilical artery, middle cerebral artery, and ductus venosus may be performed. [18]
The personnel typically required to perform an ECV include:
- Obstetrician
- Labor and delivery nurse.
ECV may only be performed in a setting where cesarean delivery services are readily available. Personnel typically required for cesarean delivery include:
- Surgical first assistant
- Anesthesia personnel
- Surgical technician or operating room nurse
- Circulating or operating room nurse
- Pediatric personnel
- Note: for cesarean delivery, labor and delivery nurses may serve as surgical technicians, circulating, or operating room roles.
- Preparation
Before attempting ECV, informed consent must be obtained; this should include tocolysis and neuraxial analgesia if those procedures will be performed. Some clinicians will obtain consent from the patient for potential emergency cesarean delivery at this time, although this practice is not universal. Additionally, an ultrasound examination should be performed to verify fetal presentation, exclude fetal and uterine anomalies, locate the placental position, and evaluate the amniotic fluid index. Many clinicians will evaluate preprocedural fetal status with a nonstress test.
The current evidence supports the administration of terbutaline 0.25mg subcutaneously 15 to 30 minutes before the ECV but does not support using calcium channel blockers or nitroglycerin for preprocedural tocolysis. [19] While multiple studies report the increased success of ECV in patients who are administered epidural or spinal neuraxial anesthesia, overall data is insufficient to warrant a universal recommendation; neuraxial anesthesia may improve success rates for ECV in situations where tocolysis alone was unsuccessful. [20]
- Technique or Treatment
The gravida should be supine with a leftward tilt using a wedge support to relieve pressure on the great vessels. ECV is best performed using a 2-handed approach.
If the fetal presentation is breech, lift the breech out of the pelvis with one hand and apply downward pressure to the posterior fetal head to attempt a forward roll. If a forward roll is unsuccessful, a backward roll can be attempted. If the fetus is in either a transverse or oblique presentation, similar manipulation of the fetus is used to try to move the fetal head to the pelvis. [21]
Fetal well-being should be evaluated intermittently with Doppler or real-time ultrasonography during ECV. ECV should be abandoned if there is significant fetal bradycardia, patient discomfort, or if a version is not achieved easily. After a successful or unsuccessful ECV, external fetal heart rate monitoring should be performed for 30 to 60 minutes. If the gravida is Rh negative, anti-D immune globulin should be administered.
Immediate induction of labor to minimize reversion is not recommended. If the initial attempt at ECV is unsuccessful, additional attempts can be made during the same admission or at a later date.
- Complications
Complications of ECV are rare and occur in only 1% to 2% of attempts. The most common complication associated with ECV is fetal heart rate abnormalities, particularly bradycardia, occurring at a rate of 4.7% to 20%; these abnormalities usually are transient and improve upon completion or abandonment of the procedure.
More severe complications of ECV occur at a rate of less than 1% and include premature rupture of membranes, cord prolapse, vaginal bleeding, placental abruption, fetomaternal hemorrhage, emergent cesarean delivery, and stillbirth. Many of these rare complications require emergent cesarean delivery; some clinicians choose to perform ECV in the operating room, although this is neither necessary nor universal. [22]
ECV is associated with changes in Doppler indices that may reflect decreased placental perfusion. It appears these changes are short-lived and have no detrimental effects on the outcomes of uncomplicated pregnancies. A recent prospective study investigating the effects of ECV on fetal circulation in the antepartum period noted no differences in the Doppler evaluation of the middle cerebral artery or ductus venosus; all studied patients remained stable and were discharged home after the procedure. [18]
- Clinical Significance
Some data indicate that only 20% to 30% of eligible candidates are offered ECV. [23] Patients who undergo a successful ECV procedure have a lower cesarean delivery rate than patients who do not but are still at a higher risk of cesarean delivery than patients with cephalic fetuses who do not require ECV. ECV is cost-effective if the probability of a successful ECV exceeds 32%. Overall, ECV is successful in 58% of attempts, reduces the risk for CS by two-thirds, and enables 80% of these patients to deliver vaginally. [24]
- Enhancing Healthcare Team Outcomes
ECV is not a benign procedure and is most successful when performed under the care of an interprofessional team. Labor and delivery nurses play an integral role in the success of ECV as they frequently assist in the procedure, prepare the patient for ECV, and implement external fetal monitoring before, during, and after the procedure. Additionally, the support of emergent operating room staff promotes the safe delivery of a healthy fetus should complications arise during the ECV procedure. Clear and concise anticipatory interprofessional communication improves safety and outcomes for the gravida and the fetus should complications occur.
- Review Questions
- Access free multiple choice questions on this topic.
- Comment on this article.
Disclosure: Meaghan Shanahan declares no relevant financial relationships with ineligible companies.
Disclosure: Daniel Martingano declares no relevant financial relationships with ineligible companies.
Disclosure: Caron Gray declares no relevant financial relationships with ineligible companies.
This book is distributed under the terms of the Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International (CC BY-NC-ND 4.0) ( http://creativecommons.org/licenses/by-nc-nd/4.0/ ), which permits others to distribute the work, provided that the article is not altered or used commercially. You are not required to obtain permission to distribute this article, provided that you credit the author and journal.
- Cite this Page Shanahan MM, Martingano DJ, Gray CJ. External Cephalic Version. [Updated 2023 Dec 13]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2024 Jan-.
In this Page
Bulk download.
- Bulk download StatPearls data from FTP
Related information
- PMC PubMed Central citations
- PubMed Links to PubMed
Similar articles in PubMed
- Value of routine ultrasound examination at 35-37 weeks' gestation in diagnosis of non-cephalic presentation. [Ultrasound Obstet Gynecol. 2020] Value of routine ultrasound examination at 35-37 weeks' gestation in diagnosis of non-cephalic presentation. De Castro H, Ciobanu A, Formuso C, Akolekar R, Nicolaides KH. Ultrasound Obstet Gynecol. 2020 Feb; 55(2):248-256.
- External cephalic version at 38 weeks' gestation at a specialized German single center. [PLoS One. 2021] External cephalic version at 38 weeks' gestation at a specialized German single center. Zielbauer AS, Louwen F, Jennewein L. PLoS One. 2021; 16(8):e0252702. Epub 2021 Aug 30.
- External cephalic version in singleton pregnancies at term: a retrospective analysis. [Gynecol Obstet Invest. 2008] External cephalic version in singleton pregnancies at term: a retrospective analysis. Zeck W, Walcher W, Lang U. Gynecol Obstet Invest. 2008; 66(1):18-21. Epub 2008 Jan 30.
- Review [Breech Presentation: CNGOF Guidelines for Clinical Practice - External Cephalic Version and other Interventions to turn Breech Babies to Cephalic Presentation]. [Gynecol Obstet Fertil Senol. 2...] Review [Breech Presentation: CNGOF Guidelines for Clinical Practice - External Cephalic Version and other Interventions to turn Breech Babies to Cephalic Presentation]. Ducarme G. Gynecol Obstet Fertil Senol. 2020 Jan; 48(1):81-94. Epub 2019 Oct 31.
- Review Association between hospitals' cesarean delivery rates for breech presentation and their success rates for external cephalic version. [Eur J Obstet Gynecol Reprod Bi...] Review Association between hospitals' cesarean delivery rates for breech presentation and their success rates for external cephalic version. Athiel Y, Girault A, Le Ray C, Goffinet F. Eur J Obstet Gynecol Reprod Biol. 2022 Mar; 270:156-163. Epub 2022 Jan 13.
Recent Activity
- External Cephalic Version - StatPearls External Cephalic Version - StatPearls
Your browsing activity is empty.
Activity recording is turned off.
Turn recording back on
Connect with NLM
National Library of Medicine 8600 Rockville Pike Bethesda, MD 20894
Web Policies FOIA HHS Vulnerability Disclosure
Help Accessibility Careers
Cephalic presentation at 32 weeks

You May Also Like
Planning visitors during hospital stay, you’re pregnant how these moms reacted, jump to your week of pregnancy, trending on what to expect, moms share home remedies for pregnancy morning sickness, 8 expensive products moms say are worth the money, ⚠️ you can't see this cool content because you have ad block enabled., 14 moms on what labor really feels like, what are your go-to healthy snacks, things they don't tell you about: mom edition, pregnancy brain moments let's have a laugh, help keep our community safe, to create a safe place, please, on our end, we will.
You and your baby at 32 weeks pregnant
Your baby at 32 weeks.
By about 32 weeks, the baby is usually lying with their head pointing downwards, ready for birth. This is known as cephalic presentation.
If your baby is not lying head down at this stage, it's not a cause for concern – there's still time for them to turn.
The amount of amniotic fluid in your uterus is increasing, and your baby is still swallowing fluid and passing it out as urine.
You at 32 weeks
Being active and fit during pregnancy will help you adapt to your changing shape and weight gain. It can also help you cope with labour and get back into shape after the birth.
Find out about exercise in pregnancy .
You may develop pelvic pain in pregnancy. This is not harmful to your baby, but it can cause severe pain and make it difficult for you to get around.
Find out about ways to tackle pelvic pain in pregnancy .
Read about the benefits of breastfeeding for you and your baby. It's never too early to start thinking about how you're going to feed your baby, and you do not have to make up your mind until your baby is born.
Things to think about
- how you might feel after the birth
Start4Life has more about you and your baby at 32 weeks pregnant .
You can sign up for Start4Life's weekly emails for expert advice, videos and tips on pregnancy, birth and beyond.
Page last reviewed: 13 October 2021 Next review due: 13 October 2024

IMAGES
VIDEO
COMMENTS
Hi I had 20 weeks anomaly scan and there shows cephalic presentation with oblique lie . I'm worried if cephalic presentation at 20 weeks is normal or not or…
Frank breech. When a baby's feet or buttocks are in place to come out first during birth, it's called a breech presentation. This happens in about 3% to 4% of babies close to the time of birth. The baby shown below is in a frank breech presentation. That's when the knees aren't bent, and the feet are close to the baby's head.
Occiput or cephalic anterior: This is the best fetal position for childbirth. It means the fetus is head down, facing the birth parent's spine (facing backward). Its chin is tucked towards its chest. The fetus will also be slightly off-center, with the back of its head facing the right or left. This is called left occiput anterior or right ...
Most babies settle into their final position somewhere between 32 to 36 weeks gestation. Head Down, Facing Down (Cephalic Presentation) This is the most common position for babies in-utero. In the cephalic presentation, the baby is head down, chin tucked to chest, facing their mother's back. This position typically allows for the smoothest ...
Is a cephalic presentation at 20 weeks pregnancy normal? • Is your baby in the right position for birth? Find out in this informative video on cephalic prese...
The cephalic position is when a fetus is head down when it is ready to enter the birth canal. This is one of a few variations of how a fetus can rest in the womb and is considered the ideal one for labor and delivery. About 96% of babies are born in the cephalic position. Most settle into it between the 32nd and 36th weeks of pregnancy.
Cephalic presentation means a fetus is in a head-down position. Vertex refers to the fetus's neck being tucked in. There are other types of cephalic presentations like brow and face. These mainly describe how the fetus's neck is flexed. ... Most fetuses settle into a presentation around 32 to 36 weeks of pregnancy. It's possible for a ...
Presentation refers to which part of your baby's body is facing towards your birth canal. Position refers to the direction your baby's head or back is facing. Your baby's presentation will be checked at around 36 weeks of pregnancy. Your baby's position is most important during labour and birth.
I would prefer head down over breeches anytime. My 1st and 2nd were always head down early. This one is any way she feels lol, normally curled up into a ball with her feet on my bladder! My daughter was head down at our anatomy scan but then at our follow up two weeks later was Breech.
Fetal presentation, or how your baby is situated in your womb at birth, is determined by the body part that's positioned to come out first, and it can affect the way you deliver. At the time of delivery, 97 percent of babies are head-down (cephalic presentation).
A cephalic presentation or head presentation or head-first presentation is a situation at childbirth where the fetus is in a longitudinal lie and the head enters the pelvis first; the most common form of cephalic presentation is the vertex presentation, where the occiput is the leading part (the part that first enters the birth canal). All other presentations are abnormal (malpresentations ...
External Cephalic Version (ECV) External cephalic version, or ECV, is a procedure used to turn a baby from a breech position to a head-down position. It's typically done around 37 weeks of pregnancy and improves your chances of having a vaginal birth. Contents Overview Procedure Details Risks / Benefits Recovery and Outlook Additional Details.
Introduction. Cephalic presentation is the most physiologic and frequent fetal presentation and is associated with the highest rate of successful vaginal delivery as well as with the lowest frequency of complications 1.Studies on the frequency of breech presentation by gestational age (GA) were published more than 20 years ago 2, 3, and it has been known that the prevalence of breech ...
The global cesarean section rate has increased from approximately 23% to 34% in the past decade. Fetal malpresentation is now the third-most common indication for cesarean delivery, encompassing nearly 17% of cases. Almost one-fourth of all fetuses are in a breech presentation at 28 weeks gestational age; this number decreases to between 3% and 4% at term. In current clinical practice, most ...
Yes: Hi! Cephalic presentation means that the head is down which is the right position for a normal vaginal delivery. Since it's only 20th week, baby still has some room to move but most likely will not turn around. Your ob will continue monitoring baby's position because it's also important for the vertex (top of head) to be the presenting ...
00:00 - Is cephalic presentation normal at 20 weeks?00:42 - Is cephalic position good?Laura S. Harris (2020, December 31.) Is cephalic presentation normal at...
Cephalic presentation just means head down and facing your back. It does not necessarily indicate that labor will be soon without other indicators like effacement, dilation, engagement. Like. m. mintyfresh21. Jan 14, 2021 at 4:41 AM. @thencomesthree,
By about 32 weeks, the baby is usually lying with their head pointing downwards, ready for birth. This is known as cephalic presentation. If your baby is not lying head down at this stage, it's not a cause for concern - there's still time for them to turn. The amount of amniotic fluid in your uterus is increasing, and your baby is still ...
Im 38 weeks pregnant my liquor is adequate (doppler scan- fetal heart beat 124 edd 11th may18 Cephalic presentation spine to the right weight 3400) gyne has assessed chances of normal delivery z 50% as baby back is placed on the right side.. After 1 week she said now is positioned on the left side.
Cephalic presentation at 20 weeks cephalic presentation Baby kicking at 24 weeks Disclaimer : The content is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding your medical condition.